
This typically affects patients with high-risk MDS features, with a median time to transformation of 274 days from initial diagnosis. 3, 4 In some cases of MDS, a transformation to acute leukemia can take place. 2 Although it carries a link to MDS, malignancy-associated SS is most often associated with acute myelogenous leukemia (AML), with a temporal pattern revolving around the onset and relapse of underlying disease. Sweet Syndrome (SS also known as acute febrile neutrophilic dermatosis) is a systemic inflammatory disorder that is typically characterized by high fever, leukocytosis, and tender regions of erythema. 1 The wide range of disease manifestations includes persistent alterations in cell lines that cause their respective complications, and paraneoplastic syndromes. 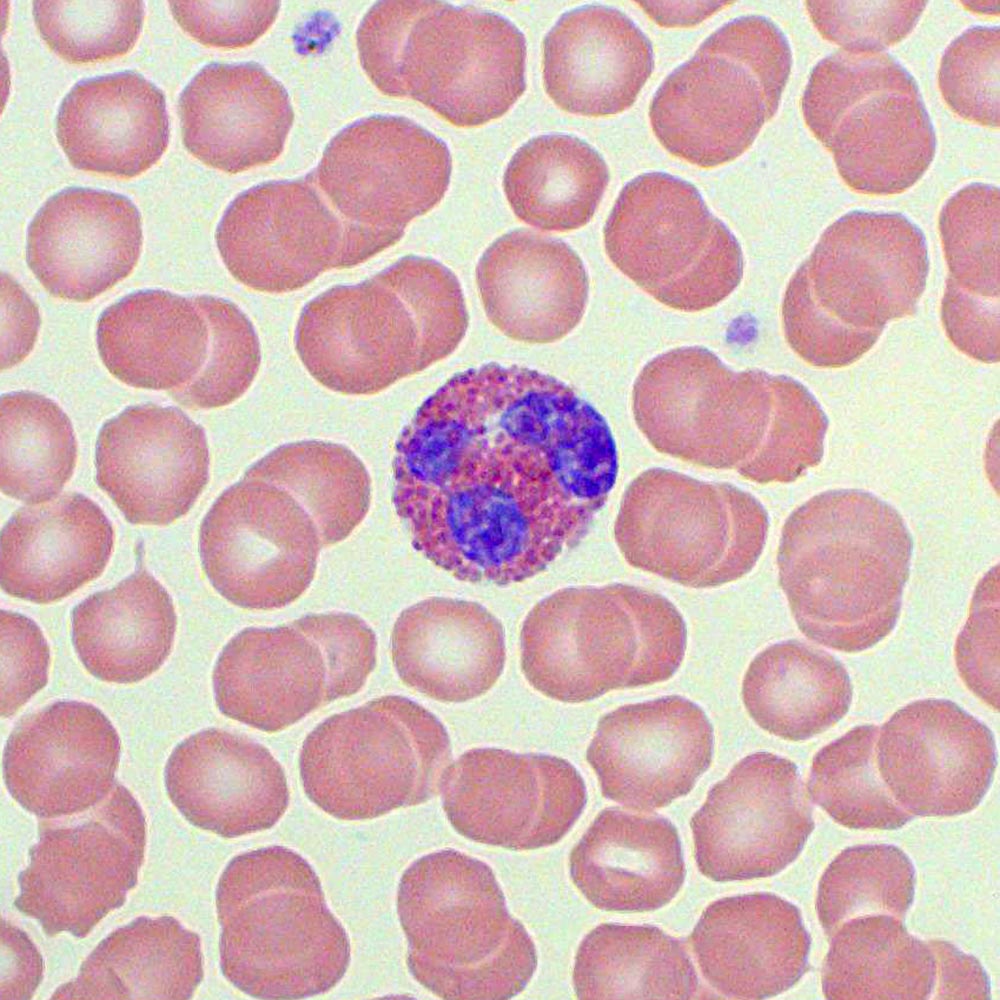
Various transforming mutations that affect hematopoietic stem cells can lead to different patterns of dysregulated signal transduction, bringing rise to phenotypic diversity. The immature granulocytes count of children, especially premature neonates or neonates younger than seven days, has to be taken with care due to their immature immune systems and the greater number of immature cells in the circulating blood.Myelodysplastic syndrome (MDS) is characterized by stem-cell-derived clonal myelopoiesis with an alteration in proliferation and differentiation. It is more useful as a monitoring parameter when the patient has already been diagnosed correctly and is under treatment. However, it can support diagnosis and prediction together with other parameters such as cytokines, interleukins and CRP. The immature granulocytes count alone does not let you predict sepsis (= when your body has an unusually severe response to an infection) or infection. However, elderly patients, neonates, and patients with myelosuppression may have elevated Immature granulocytes without an elevation of the neutrophil count. Usually an increase in Immature granulocytes is accompanied by an increase in the absolute neutrophil count. Immature granulocytes are usually not detected in healthy individuals but are elevated in patients with: Evaluation of the IG count is therefore a promising option in sepsis. The presence of immature granulocytes (IG) in the peripheral blood provides important information indicating enhanced bone marrow activity. With the exception of blood from neonates or pregnant women, the appearance of immature granulocytes in the peripheral blood indicates an early-stage response to infection, inflammation or other stimuli of the bone marrow. Immature granulocytes can be elevated in inflammatory disease IG could also be elevated in other conditions like inflammatory or cancerous diseases and in pregnancy. Immature granulocytes (IG) level in peripheral blood is used as an early sign of infection. Measurement of immature granulocytes (IG) percentage may be used as a marker of bacterial infections. More than 2% immature granulocytes is a high count. Thus, it’s an important test for patients receiving chemotherapy, diagnosed with HIV/AIDS, or ones in the ICU in the hospital. 
When this test is run, if the result shows an increase, it means that the immune response will be severe. They may already have a suppressed immune system. Immature granulocyte counts are often tests ordered for patients that are highly susceptible to develop infections. However, whenever your body is fighting an infection, it will increase its white blood cell count, and more of the white blood cells will be immature. Small amounts of white blood cells may be present on a complete blood count test whether or not you have an infection although healthy people do not show immature granulocytes on their blood test report. Immature granulocytes are white blood cells that are immature.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
